This image is © Kake L Pugh and is available for reuse under the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0) license.
The process by which new blood capillaries grow into a wound space after injury is known as angiogenesis. Wound angiogenesis is an important part of the proliferative phase of healing; in fact the term `granulation tissue' was used by John Hunter in 1787 [1] to describe the appearance of the prominent blood vessels of the initial connective tissue formed in the wound space.
Healing of any skin wound other than the most superficial cannot occur without angiogenesis. Not only does any damaged vasculature need to be repaired, but the increased local cell activity necessary for healing requires an increased supply of nutrients from the bloodstream. Moreover, the endothelial cells which form the lining of the blood vessels are important in themselves as organizers and regulators of healing.
It is interesting to note that angiogenesis also occurs in many other situations, including solid tumour growth and metastasis; rheumatoid arthritis; psoriasis; scleroderma; placental growth and embryo implantation; and three common causes of blindness - diabetic retinopathy, retrolental fibroplasia and neovascular glaucoma (in fact, diseases of the eye are almost always accompanied by vascularization [2]) [3], [4]. The process of wound angiogenesis has many features in common with tumour angiogenesis [5].
Angiogenesis proceeds concurrently with the formation of new tissue (granulation tissue), which typically begins about 4 days post-wounding [6]. It is stimulated by the chemicals (soluble factors) released by wounded tissue [7]. The resulting processes are tightly regulated by cell-cell interactions, cell-ECM interactions and cell-soluble factor interactions [7].
A blood capillary consists of a hollow tube lined with endothelial cells. The outside of the tube is covered with a layer known as the basement membrane, a major component of which is collagen IV, and which also contains fibronectin and proteoglycans (compounds consisting mainly of polysaccharides but also containing protein) [8].
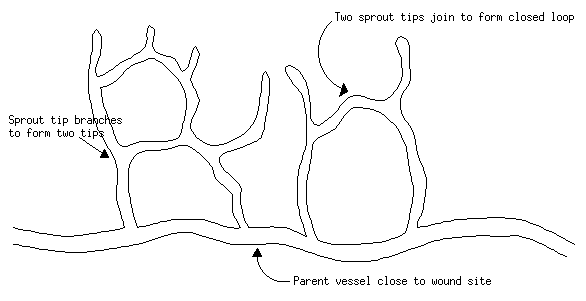
Angiogenesis begins with degradation of the basement membrane, followed by migration of endothelial cells out of the vessel. These cells then form into a tube which `sprouts' from the old capillary and is extended further into the wound space as the cells behind the leading tip begin to proliferate. The tips of such tubes can branch and eventually join up with other sprouts to form a closed loop through which blood can flow.

This image is © Kake L Pugh and is available for reuse under the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0) license.
The sprouting process begins again from these new vessels, until the wound space is permeated by a network of new capillaries. The cells of the capillaries first synthesize themselves a provisional covering containing fibronectin and proteoglycans, and finally form a true basement membrane [6, pages 18-19].
As the granulation tissue matures, most of its vessels begin to disappear [10]. The endothelial cells begin to undergo programmed cell death (apoptosis) and are removed from the tissue by scavenging macrophages [11].